
Acute care is given, often in an emergency department, when a patient has a severe but usually brief illness or condition. The medical record of the patient, both as an in-patient and later as an out-patient, should be kept up to date and include a plan of care. This record should provide an accurate, timely and ongoing record of the patient’s condition. Completeness is important in maintaining continuity of care.
Admission and Consent Records

The admission records contain all the pertinent information about the patient and include physician’s name, patient address, date of birth, consents for treatment and procedures, insurance data, Social Security number, family information and phone numbers. There will also be specific instructions about resuscitation, a Living Will, power-of attorney documents and all specific information concerning relatives to be contacted in case of emergency. If the patient is an organ donor, there will be additional documents and instructions.
History and Physical
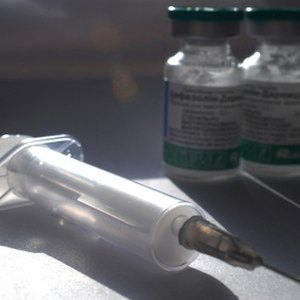
The history and physical must be completed by the physician or his designee within a specific time. It will contain information and physical findings about past illnesses and injuries, and the specific condition which has brought the patient to the hospital.
Physician's Orders

Physicians may give orders for admission and treatment before the patient arrives at the hospital. Treatment can’t begin without physician’s orders. These orders may be given over the phone to a nurse but the physician must review and sign them within a designated time. All physicians’ orders must be in writing and signed. If a nurse takes a verbal order from the doctor, it must be written on the physician’s orders record, reviewed and signed as with telephone orders. Physicians sometimes give direct orders to physical therapists but they must be incorporated into the patient’s record and signed by the prescriber.
Physician's Progress Notes

The progress notes are an ongoing record of the treatments planned and initiated, and the patient’s response to each therapy. It includes an ongoing plan of care. When a specialist is consulted, he may send a complete report of his findings later, but the consultation visit is documented in the progress notes. Ongoing specialty care, such as oncology, is documented with treatment suggestions. Surgeons, anesthetists and specialists document seeing the patient.
Nurses' Notes and Medication Records
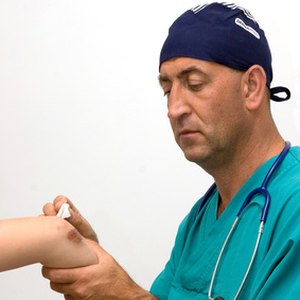
The nurses care for the patient day to day and monitor progress or decline. They document this and their observations in the “Nurses’ Notes” or nursing progress notes. These records are maintained by licensed nursing staff. The patient’s vital signs, such as blood pressure records, are maintained on separate forms by nurses and unlicensed ancillary staff. The medication record documents every dose of medication given by nurses. The parenteral fluids flow sheet records all intravenous and subcutaneous fluids administered. Licensed nursing staff maintains these records.
Ancillary Services and Consultation Records
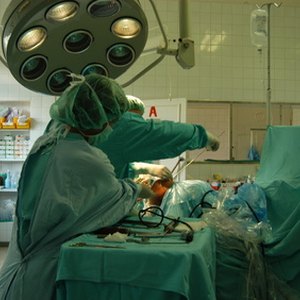
The record contains all radiologic findings, laboratory reports, surgical consultations and operative reports, pathology findings, special consultations and specialty care such as nuclear medicine or psychiatric interventions or observations. It contains records of all care and results of diagnostic procedures. A discharge summary is prepared which outlines condition, treatment, progress and prognosis.
References
Writer Bio
Nancy Williams has been writing about health-related topics since 1979. Her work has been published in "Prevention," "Nurseweek" and "Senior Life." Williams is a registered nurse with more than 35 years of experience and holds a Bachelor of Science degree in health-care administration. She is working on a book about historic sites in the West.

